Most Vendors Sell Software. Vironix Delivers Outcomes.
Unified RPM, CCM, RTM, PCM, and APCM with embedded clinical staff and end-to-end operational support.
We operate your virtual care programs so practices can scale revenue and improve outcomes without adding staff.

Unified RPM + CCM
Every virtual care service in one platform — billed automatically
Stop juggling fragmented vendors. Vironix runs RPM, CCM, RTM, PCM, CCCM, and APCM from a single workflow with embedded medical assistants doing the work.What you get
Outcomes you can measure on day 30
Each feature ties to a billable hour, an enrolled patient, or a captured CPT code — not buzzwords.
One workflow for every VCM service
RPM, RTM, CCM, PCM, CCCM, and APCM run from the same dashboard with the same staff. No vendor switching, no duplicate charts.
Built for the conditions that drive admissions
Heart Failure, COPD, Asthma, Diabetes, and CKD care plans tuned to catch decompensations before they become readmissions.
Catch decompensations before they become admissions
Risk stratification flags the patients who need a call today, so your team spends time where it changes outcomes — not chasing data.
Embedded medical assistants do 95% of the work
We staff the monitoring, the outreach, and the documentation. Your providers see the revenue without the operational lift.
Automated CPT capture and audit-ready claims
Every minute, every reading, every CPT code logged automatically. Submit faster, get paid sooner, defend against audits.
Patients stay enrolled — 93% of them
In-person enrollment, cellular devices, and proactive outreach drive industry-leading retention. Enrollment is the whole game.
Outcomes, not features
Why practices switch to Vironix
Side-by-side outcomes vs. fragmented RPM-only and CCM-only vendors.
- Enrollment rate
- ~15%
- Annual revenue per provider
- $15–30K
- Who does the work
- You and your staff
- RPM coverage
- Yes
- CCM coverage
- No
- Implementation
- 60–90 days
- Upfront cost
- $10K+
- Enrollment rate
- Varies
- Annual revenue per provider
- $20–40K
- Who does the work
- Remote-only team
- RPM coverage
- No
- CCM coverage
- Yes
- Implementation
- 30–60 days
- Upfront cost
- Setup fees
- Enrollment rate
- 93%
- Annual revenue per provider
- $300K
- Who does the work
- We do 95% of the work
- RPM coverage
- Yes — unified
- CCM coverage
- Yes — unified
- Implementation
- 30 days
- Upfront cost
- $0
The revenue math
$300K annual profit per provider
Real billing, not theoretical
Unified RPM + CCM stacks revenue per patient
Bill the codes you already qualify for and the ones fragmented vendors leave on the table. Same patient, same visit, more revenue.
More revenue than any RPM-only competitor
Higher enrollment + broader code coverage = a profit-per-provider number that competitors cannot match.
Claim-ready documentation and billing partner support
We track time, organize CPT-ready documentation, generate billing reports, and coordinate with your billing team or trusted billing partners so claims can be submitted cleanly.
How it actually works
Built for outcomes, validated by science
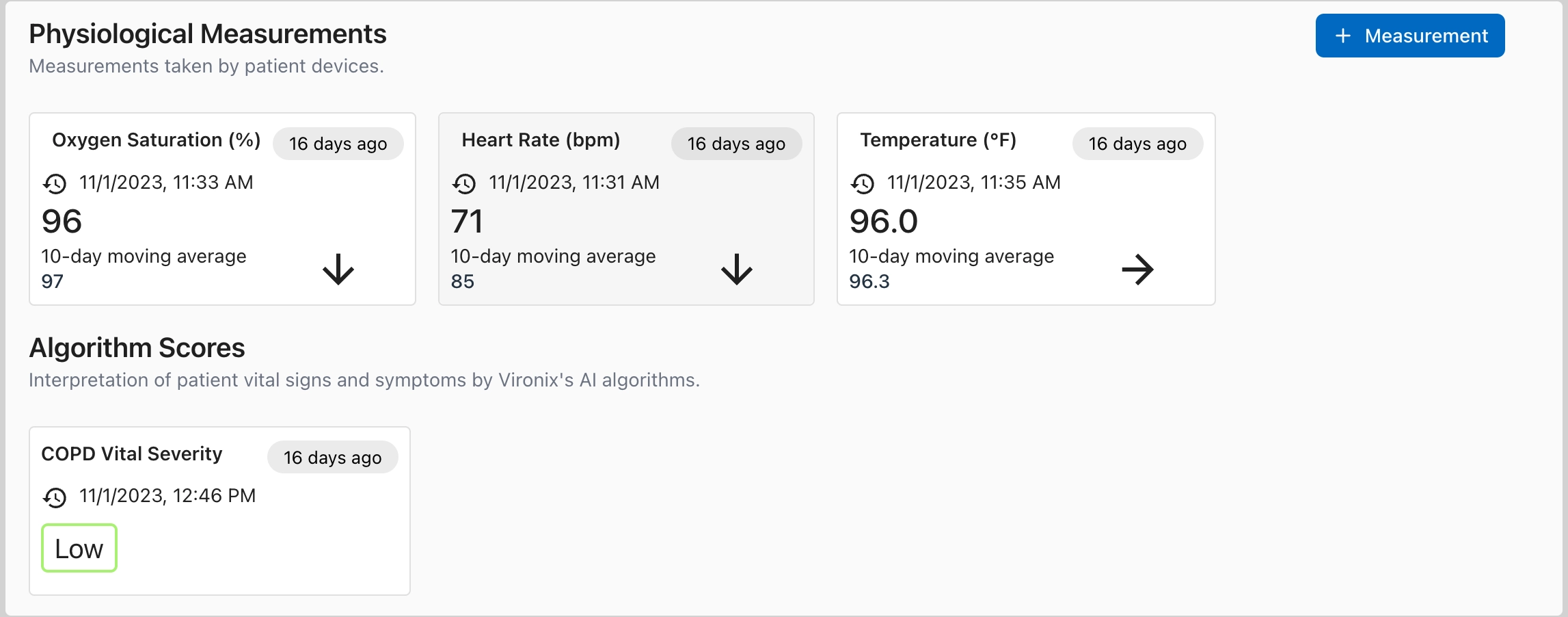
Patient-friendly devices, in-person enrollment, embedded MAs, and risk models that catch what matters — published in peer-reviewed journals.Patient mobile app and self-assessments
Patients see their data and answer condition-specific check-ins, so your team gets actionable signal between visits.
Cellular devices, no setup needed
Oximeters, BP cuffs, weight scales, glucometers, and spirometers ship cellular-ready. Patients use them out of the box — no app pairing.
In-person enrollment drives the 93%
We screen for qualified patients and enroll them in person. That is how enrollment goes from 15% to 93%.
Risk stratification that catches decompensations
Clinically validated models flag patients heading toward an adverse event so your team intervenes early. Research published, not promised.
30-day implementation. $0 upfront.
No integrations to wait on, almost no staff time required, no upfront cost — start billing in 30 days.
Step 1: Discovery (Day 0)
30-minute call to confirm fit, map your patient population to billable codes, and project your revenue.
Step 2: Sign and ship (Days 1–7)
Agreements signed, devices shipped, embedded MAs assigned, billing pathway finalized.
Step 3: Enroll and monitor (Days 7–30)
We enroll patients in person and start monitoring. Your team keeps doing what it does — we handle the rest.
Step 4: Submit claims (Day 30)
Claim-ready reports are generated for your billing team or billing partner. Revenue can begin in the first month.
Outcomes — answered straight
Built for your practice
Who Vironix is built for
Different practices, different pains — same outcome: more revenue, less operational lift.
Revenue generation, staff burden, patient engagement.
Add $300K profit per provider. We handle operations — you focus on clinical.
System integration and efficiency across the network.
Scale RPM + CCM across your system. Embedded MAs cut administrative burden.
Managing a broad panel plus targeted high-risk chronic patients across multiple billing pathways.
APCM for most of the panel, RPM and CCM for targeted chronic-illness patients — billed correctly per patient, all in one workflow.
Specialty-specific RPM opportunities (post-op, high-risk).
Maximize RPM revenue in your specialty. 93% enrollment.
Frequently asked questions
See your number on a 30-minute call
We will model the profit-per-provider for your patient population. Zero upfront cost. 30 days to first claim.